Frequently Asked Questions About Cholesteatoma
What Is a Cholesteatoma?
A cholesteatoma is a skin cyst that occurs in the middle ear.
When certain risk factors are present, the ear drum becomes floppy and retracted. This creates a pocket in the middle ear that collects skin cells and skin debris.
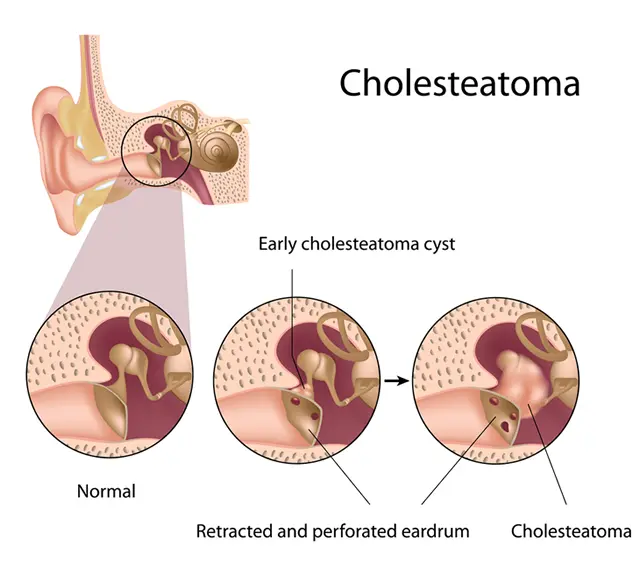
What Causes a Cholesteatoma?
Certain risk factors create a favorable situation for cholesteatoma in your ear.
These include recurrent ear infections, chronic allergies, cigarette smoke, Eustachian tube dysfunction, and congenital abnormalities.
How Would I Know if I Have a Cholesteatoma?
Symptoms that may indicate a cholesteatoma include hearing loss, recurring ear infections, and drainage from the ear canal.
The drainage may have a bad smell. It may also be discolored. Rarely, some cholesteatomas do not have symptoms and are noted on routine ear exam.
What Should I Do if I Am Concerned?
Visit your doctor.
These symptoms do not necessarily indicate a cholesteatoma, but your physician can exam your ear. In addition, they may recommend medical treatment, a hearing test, and a referral to an ear specialist.
Do I Need to See an Ear Specialist (Neurotologist)?
You should see someone trained in ear surgery.
Although symptoms of cholesteatoma will respond to medical treatments such as antibiotics given by mouth or by ear drop, after treatment is completed symptoms will return. No medical treatment is available to reverse the changes seen in ears with cholesteatoma, and they usually need to be removed.
Why Do They Need to Be Removed?
If left untreated, cholesteatomas will continue to grow.
As they enlarge, they damage the hearing bones resulting in worsening hearing loss. Further growth may damage the inner ear or balance system causing deafness or vertigo. Cholesteatomas that are allowed to grow many years can even destroy bone between the ear and brain leading to spinal fluid leak, herniated brain tissue, or meningitis.
How Are They Removed?
An ear specialist who has surgical training in the delicate structures of the ear removes it during day surgery.
In a procedure known as tympanoplasty with mastoidectomy, the surgeon will remove the cholesteatoma. They will also repair the damage to the ear drum and hearing bones done by the cholesteatoma. This takes around 2 hours to complete.
Is This Operation Risky?
Tympanoplasty with mastoidectomy is common.
It is usually performed in the outpatient setting, so you can go home the next day. The main risk of surgery is recurrence of cholesteatoma, so your surgeon must be very thorough. Even when cholesteatomas are completely removed, a new cholesteatoma can form if risk factors are not changed. In cases of extensive cholesteatoma, a second operation may be needed to ensure no residual cholesteatoma was left behind. Hearing loss, dizziness, and injury to structures surrounding the ear are rare risks to surgery as well.
How Is the Operation Made Safer?
CT scanning and facial nerve monitoring can make it safer.
In complex cases, CT scan is ordered before surgery to help predict variations in the surrounding structures and avoid injury. Also, facial nerve monitoring is used to enhance the safety of working around the facial nerve.
How Long Does It Take to Recover From Surgery?
Generally, one to two days off work are needed to feel normal.
After that, you will typically have a postoperative appointment within 2 weeks of the operation. You avoid getting the ear wet until cleared by your surgeon. This usually takes about 6 weeks. You should not fly during this time. Hearing improves slowly over the 2 months following surgery.
How Do I Make an Appointment?
At the Dallas Ear Institute, there are three experienced ear specialists. Please call Call (469) 803-5555 to schedule an appointment.

